In general, billing companies face many challenges with their clients due to the shortage of skill sets and domain expertise resulting in outstanding revenues and chaotic revenue cycle management.
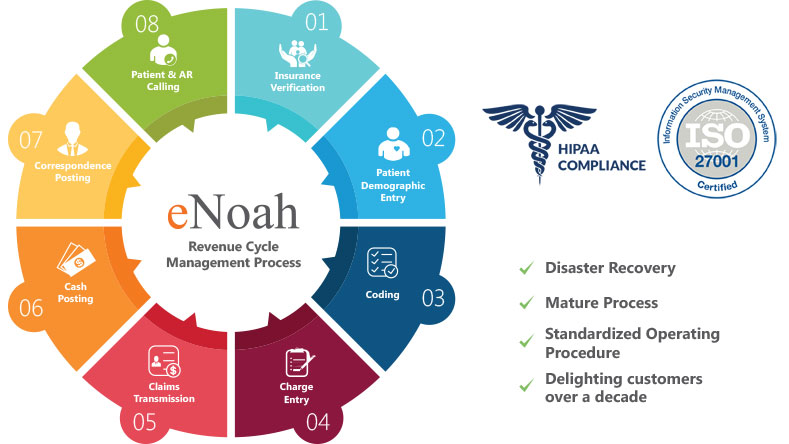
eNoah provides a wide range of services in health care RCM to physician groups and hospitals
A customer-focused Revenue Cycle Management partner with over a decade of experience delighting clients, eNoah offers unique engagement models that fit your specific needs.
Our team of competent & experienced specialists strives hard to deliver great quality in a timely & consistent manner. eNoah is HIPAA compliant & ISO 27001 Certified.
Value Proposition
With years of productive efficiency under their belts, our teams perform revenue cycle management functions with laser precision, guaranteeing reliable results that allow our partners to achieve sustained growth by focusing on their core business functions and eliminating time and cost waste.
- RCM specialists with experience in handling diverse specialties
- Professionals with experience in handling various medical billing applications
- Experienced AR analysts and denial management specialists
- Significant savings in process cost
- Better utilization of client’s high value resources