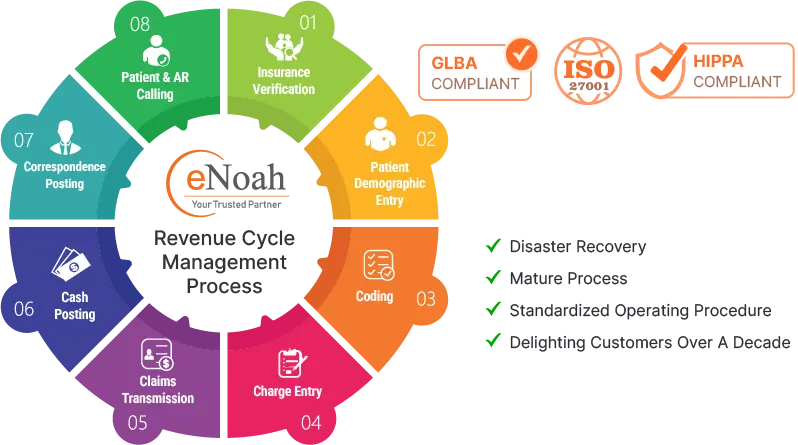
Revenue Cycle Management Services
End-to-end revenue cycle management services including Patient Demographics Entry, Insurance Verification Process, Charge Entry Services, Electronic Claim Submission, Cash Posting, Denial Management, Patient Billing, Accounts Receivable Management, and Follow Up.